Dialysis
Dialysis is an artificial process that uses filtering machine or a special fluid in your belly to filter waste out of your body. It is typically needed when approximately 90% or more of kidney function is lost. When the kidneys fail, your body may have difficulty filtering out the waste products and keeping a chemical balance. Dialysis rids your body of waste, toxins, and excess fluid by filtering the blood.
In some cases, dialysis may only be needed for a short time until the kidneys heal. As the kidneys lose their ability to function, waste products begin to build up in the blood. Patients usually need dialysis when the waste products in their body become so high that their body cannot maintain proper electrolyte balance. Dialysis only filters out waste; it can’t replace other functions of the kidney. It helps control blood pressure and keeps the electrolytes in balance.
It can be performed at home or in a hospital by trained healthcare professionals. If they choose to do home dialysis, special training will be provided to the patient and the partner. The two types of dialysis, hemodialysis and peritoneal dialysis use different methods to filter blood.
Hemodialysis
Hemodialysis is a mechanical process to clean the blood of waste products. In hemodialysis, an external machine filters wastes, salts and fluid from the blood. The blood is circulated through the dialysis machine and cleaned before being returned to the body. It is usually performed several times a week and lasts for 4-5 hours. During treatment, you may sit, sleep, read, and even work.
Procedure
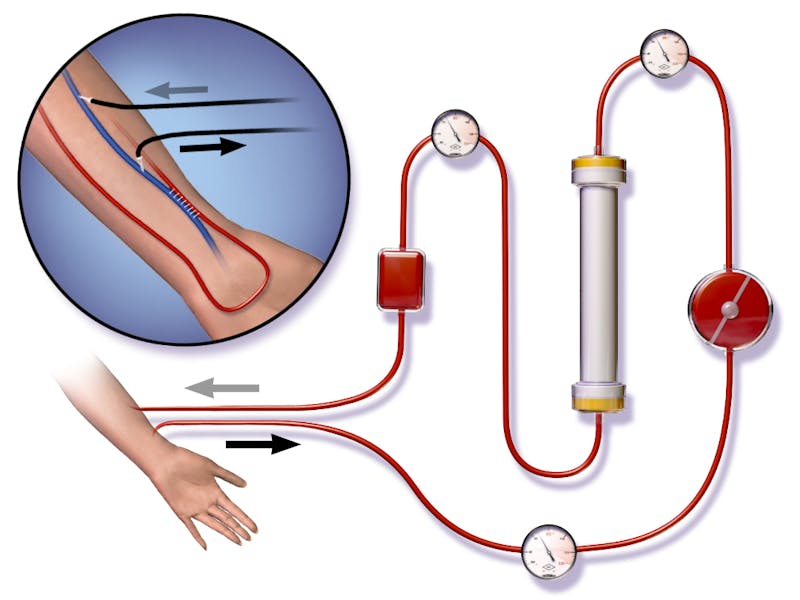
For hemodialysis, there needs to be an access point in the patient’s body to get the blood from the body to the dialyzer and back into the body. A particular type of access called an arteriovenous (AV) fistula is created surgically in the arm. This is produced by connecting an artery to a vein. This surgical connection of the artery and vein causes increased blood flow, which stimulates the size and thickness of the fistula. The access is inside the body and cannot be seen from the outside. Two needles are inserted into this access. Blood flows out of the body through one needle, circulates through the dialysis machine and flows back into the access through the other needle. If needle insertion is painful, some anesthetic ointment or spray may be applied. Sometimes, a patient’s arm veins are not suitable for creating a fistula. In this case, an alternative procedure known as AV graft may be recommended. In the AV graft, a surgeon uses a flexible, rubber-like tube to create a path between an artery and vein.
Once the patient is connected to the machine, the machine drains the blood, bathes it in a unique dialysate solution, gets it filtered and then returns it to the body.
Dialysate
Dialysate is the fluid that helps remove unwanted products from the body. Fresh dialysate from the machine enters your dialyzer throughout the treatment. The primary function of the dialysate is to remove waste material from the blood and to keep useful material from leaving the blood. Electrolytes and water are some materials included in the dialysate so that their level in the blood can be maintained.
What happens during hemodialysis?
During hemodialysis, the actual filtering happens in a part of the machine called a dialyzer or artificial kidney. The dialyzer is a hollow plastic tube that contains many tiny filters. It has two parts: one part for blood and other for dialysate. These two parts are separated by a semi-permeable membrane to prevent mixing. The membrane allows dialysate and waste to pass through, but does not allow blood to pass through. Blood cells and other vital parts of blood are too big to pass through it. Wastes are filtered out of the blood into the dialysate. Dialysate containing unwanted waste products and excess electrolytes leave the dialyzer and are washed down the drain, while the cleaned blood goes back into the body.
Complications
Possible complication of hemodialysis include:
- Cramps
- Hypotension
- Shortness of breath
- Bleeding from the access point
- Nausea and vomiting
Peritoneal dialysis (PD)
Peritoneal dialysis is a way to remove waste products from the blood when kidneys can no longer do their job adequately. It is a treatment for kidney failure that uses the thin lining of the abdomen called peritoneum to filter the blood inside the body. Dialysate fluid is circulated into the peritoneal cavity either manually or by using a machine called a cycler. The solution is allowed to remain in the abdomen for 4-6 hours before it is drained and replaced with a new PD solution. It takes about 30 minutes. This process of replacement of new PD solution with the used PD solution is called an exchange.
It does not cure the kidney disease; instead, it replaces the function of the kidney. Therefore it must continue indefinitely unless you get a kidney transplant. It is performed at home and should be done at least four to six times a day. It is important to organize the schedule at home and work to accommodate your treatment.
Preparation
Few weeks before the peritoneum dialysis starts; surgeon places a soft tube, called a catheter in the belly. It is held in place with stitches for two weeks so that the area can heal. The dressing will be done over the catheter site to promote healing and prevent infection. About 2-3 week later, the catheter will be ready for use. You will be taught how to perform exchange procedures.
Procedure
A plastic tube called a peritoneal dialysis catheter is placed through the abdominal wall into the abdominal cavity. A special sterile fluid called dialysate is introduced into the abdomen through the catheter. The fluid contains a type of sugar that draws out waste and extra fluid. Dialysate remains in the abdomen for a specified amount of time (dwell time) where it absorbs waste and extra fluid from the body. The lining of the abdomen acts as a membrane to allow excess fluids and waste products to pass from the bloodstream into the dialysate. After a few hours, the solution is drained out of the body into the empty bag. The peritoneal cavity is then refilled with fresh dialysate, and the process starts again. In between fluid changes, patient can carry out their normal activities. This process need to be repeated 4-6 times a day. The no of exchanges and amount of dwell time depends on the method of PD used.
Peritoneum
Peritoneum is a thin membrane that lines the inner surface of the abdomen. It has a rich supply of tiny blood vessels called capillaries. It works as a filter as the wastes are pulled through it.
There are two kinds of peritoneal dialysis. Both involve the use of a catheter and special PD fluid to clean the blood.
- Continuous Ambulatory Peritoneal Dialysis (CAPD) - In CAPD, the patient is not connected to any kind of machine. It is the most portable type of dialysis and involves three steps- Filling, Dwelling and Draining.
- Automated Peritoneal Dialysis (APD) - APD is an automatic process that uses a machine to perform the exchange. In APD a device called “cycler” will change the dialysate solution during the night, usually when patients are asleep.
Benefits
There are various benefits of peritoneal dialysis:
- Painless - Unlike hemodialysis, PD involves no needling. Hence it involves no pain.
- Comfort- Since it can be done at home, there is no need to travel to the dialysis centre.
- Portable- Easy to carry.
- You can perform the process at home without any assistance.
- You have the freedom to work, eat and drink more of what you like.
Risks
- Peritonitis- It is a common concern with PD. Peritonitis is an infection that affects the lining of the peritoneum. It may occur due to the permanent placement of the tube and is a common reason for the failure of PD.
- Peritoneal Dialysis is not recommended for people who are in a poor state of health. For example, in people with dementia.
- Local skin infection at the site of the catheter is also common.
DISCLAIMER
This web page provides general information and discussions about health, medicine and related subjects. The information and other content provided on this website, or in any linked materials, are not intended and should not be construed as medical advice, nor is the information a substitute for professional medical expertise or treatment.
The content is for information purpose only and is not a medical advice. Qualified doctors have gathered information from reputable sources; however Credence Medicure Corporation is not responsible for errors or omissions in reporting or explanations. No individual should use the information, resources and tools contained herein to self diagnose or self treat any medical condition.
If you or any other person has a medical concern, you should consult with your health care provider or seek other professional medical treatment. Never disregard professional medical advice or delay in seeking it because of something that have read on this blog or in any linked materials. If you think you may have a medical emergency, call your doctor or emergency services immediately.
The opinions and views expressed on this blog and website have no relation to those of any academic, hospital, health practice or other institution. Credence Medicure Corporation gives no assurance or warranty regarding the accuracy, timeliness or applicability of the content.
